Benefits of Dental Implants: How They Enhance Life and Confidence
Nearly 120 million Americans are missing at least one tooth, and by age 65, that number jumps to 25% who've lost all their natural teeth. What's particularly striking is how this impacts more than just eating—research from the American Dental Association shows that tooth loss significantly affects self-esteem, social interactions, and overall quality of life in ways that extend far beyond oral health.
The dental restoration landscape has transformed dramatically over the past decade. Where removable dentures once dominated tooth replacement options, dental implant technology has evolved to offer something fundamentally different: permanent, stable solutions that integrate directly with your jawbone (https://www.dentistsoflasvegas.com/services/dental-implants). This isn't just about aesthetics or convenience—it's about preserving the structural integrity of your facial features and maintaining the biological processes that keep your mouth healthy.
Here's what makes this particularly relevant now: as our understanding of the connection between oral health and overall wellness deepens, the stakes for tooth replacement decisions have risen considerably. The choice between traditional dentures, bridges, and implants affects not just immediate comfort, but long-term bone health, adjacent teeth preservation, and quality of life for decades to come.
Understanding how dental implants work—and why they're increasingly becoming the gold standard for tooth replacement—reveals why this technology represents such a significant advancement in restorative dentistry.
What Are Dental Implants and How Do They Work?
Definition and Core Characteristics
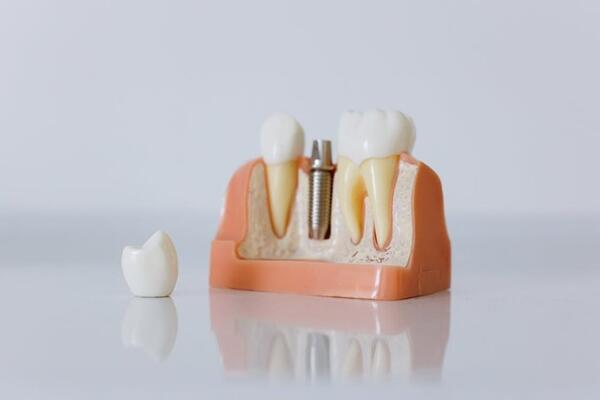
Dental implants function as artificial tooth roots, typically made from biocompatible titanium or ceramic materials that are surgically placed into the jawbone. Unlike dentures that rest on the gums or bridges that rely on adjacent teeth for support, implants create an independent foundation that doesn't compromise surrounding structures.
The critical distinction lies in how implants interact with your body. Rather than simply replacing the visible portion of a missing tooth, they restore the entire tooth structure—both the crown you see and the root that provides stability. This comprehensive approach addresses the root cause of many problems associated with tooth loss, particularly the progressive bone deterioration that occurs when natural tooth roots are absent.
What sets implants apart from other tooth replacement options is their ability to stimulate the jawbone through normal chewing forces. Your natural teeth transmit these forces through their roots, signaling the bone to maintain its density and structure. Implants preserve this crucial biological process in a way that dentures and bridges simply cannot.
Biological Process of Osseointegration
The science behind dental implant success centers on a process called osseointegration—literally meaning "bone integration." When a titanium implant is placed into the jawbone, the surrounding bone tissue gradually grows around and fuses with the implant surface over a period of three to six months.
This biological fusion occurs because titanium has a unique property: it's osteoconductive, meaning it encourages bone growth rather than triggering a foreign body rejection response. The bone cells, called osteoblasts, deposit new bone tissue directly onto the implant surface, creating a structural bond that's often stronger than the connection between natural teeth and bone.
During the healing period, the implant becomes increasingly stable as new bone formation progresses. Microscopic examination reveals bone growing into the textured surface of the implant, creating what's essentially a permanent biological weld. This process explains why implants can handle the same biting forces as natural teeth—they're literally part of your skeletal structure.
The success of osseointegration depends on several factors: adequate bone density at the implant site, proper surgical technique, and maintaining optimal healing conditions during the integration period. Understanding this process helps explain both the remarkable success rates of modern implants and the importance of proper patient selection and aftercare.
Types of Dental Implant Materials and Procedures
Advantages of Titanium and Ceramic Implants
Titanium implants remain the industry standard, backed by over 50 years of clinical research and success rates exceeding 95%. Titanium's biocompatibility is unmatched—it's the same material used in orthopedic joint replacements and has proven long-term stability in the human body. The material's strength-to-weight ratio allows for smaller implant designs while maintaining durability under significant chewing forces.
Recent advances in titanium implant surfaces have improved osseointegration rates and reduced healing times. Modern implants feature micro-textured surfaces that increase the contact area between bone and implant, accelerating the integration process. Some titanium implants now incorporate surface treatments that promote faster bone growth, reducing the typical healing period from six months to as little as three months in optimal conditions.
Ceramic implants, specifically those made from zirconia, offer distinct advantages for certain patients. Zirconia is tooth-colored, eliminating any potential for gray shadowing through the gums—a consideration particularly important in the aesthetic zone of the front teeth. These implants are also metal-free, addressing concerns for patients with metal sensitivities or those preferring biocompatible alternatives to titanium.
However, ceramic implants require more precise handling during surgery due to their brittleness compared to titanium. They're also newer to the market, with long-term data still accumulating. Current research suggests excellent biocompatibility and osseointegration rates comparable to titanium, but the track record is shorter.
Overview of the Dental Implant Surgery Process
The implant placement process typically unfolds in carefully orchestrated phases designed to optimize healing and long-term success. Initial treatment planning involves detailed 3D imaging to assess bone density, nerve locations, and optimal implant positioning. This digital planning phase often uses cone beam CT scans that allow surgeons to virtually place implants before surgery, increasing precision and reducing complications.
During the surgical phase, the implant is placed into a precisely prepared site in the jawbone. Modern techniques often allow for immediate placement following tooth extraction, reducing the total treatment time. The surgery itself is typically performed under local anesthesia, though sedation options are available for anxious patients.
Following implant placement, a healing cap is often placed to shape the gum tissue during osseointegration. After the integration period—typically three to six months—the final restoration process begins. This involves taking impressions and fabricating the crown, bridge, or denture that will attach to the implant. The entire process, from initial consultation to final restoration, usually spans four to eight months, depending on individual healing rates and complexity.
Advanced techniques like guided surgery use computer-planned surgical guides to place implants with millimeter precision, often reducing surgery time and improving outcomes. Some cases even allow for immediate loading, where a temporary crown is placed the same day as implant surgery, though this approach requires specific conditions and careful case selection.
How Dental Implants Improve Quality of Life
Functional Benefits Compared to Dentures and Bridges
The functional superiority of dental implants becomes immediately apparent when comparing bite force capabilities. Natural teeth can generate bite forces of 150-250 pounds per square inch, while implants can restore 80-90% of this capacity. Traditional dentures, by contrast, typically provide only 25-30% of natural bite force due to their reliance on gum support and suction retention.
This dramatic difference in chewing efficiency translates to real-world dietary freedom. Patients with implants can comfortably eat challenging foods like corn on the cob, apples, nuts, and tough meats—foods that denture wearers often avoid. Clinical studies demonstrate that implant patients show significantly improved nutritional status compared to denture wearers, who often shift toward softer, more processed foods that may lack essential nutrients.
Stability represents another crucial functional advantage. Dental bridges, while more stable than dentures, require the removal of healthy tooth structure from adjacent teeth to serve as anchors. This compromises the long-term health of supporting teeth and creates potential failure points. Implants eliminate this compromise, functioning independently without affecting neighboring teeth.
The impact on daily activities extends beyond eating. Denture wearers frequently experience slipping, clicking, or the need for adhesives that can affect speech patterns and social confidence. Implants eliminate these concerns entirely, providing the same stability and reliability as natural teeth during speaking, laughing, and other social interactions.
Impact on Facial Structure and Bone Preservation
Perhaps the most significant long-term benefit of dental implants lies in their ability to preserve facial bone structure. When natural teeth are lost, the alveolar bone that once supported them begins to resorb—a process that can result in 25% bone loss in the first year alone. This resorption continues throughout life, gradually changing facial dimensions and creating the sunken appearance often associated with aging.
Traditional dentures accelerate this bone loss process. The pressure from dentures actually stimulates bone resorption, creating a cycle where dentures become progressively looser as the underlying bone shrinks. This explains why denture wearers often require relines, adjustments, and eventual replacement as their facial structure changes.
Implants interrupt this destructive cycle by providing the mechanical stimulation that bones need to maintain their density. Each time you chew, the forces transmitted through the implant signal the surrounding bone to remain active and strong. Research published in the Journal of Periodontology shows that areas with dental implants maintain bone density at levels comparable to natural teeth, even decades after placement.
The facial support provided by implants also preserves the natural contours of your lips and cheeks. This maintenance of facial height and volume contributes to a more youthful appearance and prevents the premature aging that often accompanies extensive tooth loss. The psychological benefits of maintaining facial aesthetics often prove as valuable to patients as the functional improvements.
Speech and Chewing Efficiency Improvements
Clear speech depends heavily on the precise positioning of teeth and tongue during sound formation. Missing teeth, particularly in the front areas, can create lisping, whistling, or difficulty pronouncing certain consonants. Ill-fitting dentures compound these problems by shifting during speech or requiring conscious effort to keep them in place.
Implants restore the natural landscape of your mouth, providing the proper support for tongue positioning and airflow needed for clear speech. Unlike dentures, which can create a bulky feeling that affects tongue movement, implants feel and function like natural teeth. Patients report that speech improvements often occur immediately after the final restoration is placed, with complete adaptation typically occurring within days.
The precision of implant placement also allows for optimal crown contours that support proper lip and cheek positioning during speech. This attention to detail during the restoration phase ensures that implants not only function well mechanically but also provide the subtle support structures that contribute to natural speech patterns.
Chewing efficiency improvements extend beyond simple bite force measurements. The proprioception—your body's awareness of tooth position and pressure—remains largely intact with implants due to their direct bone connection. This sensory feedback allows for more controlled and efficient chewing, reducing the risk of accidentally biting the tongue or cheek that denture wearers sometimes experience.
Risk Factors and Patient Eligibility for Dental Implants
Common Complications and Causes of Implant Failure
While dental implants boast success rates exceeding 95%, understanding the factors that contribute to the 5% failure rate helps ensure optimal outcomes. Early implant failure typically occurs within the first few months and usually relates to osseointegration problems. This can result from inadequate bone quality, surgical trauma, infection, or premature loading of the implant before integration is complete.
Late implant failure, occurring months or years after placement, most commonly stems from peri-implantitis—essentially gum disease around the implant. This condition develops when bacterial plaque accumulates around the implant, causing inflammation and eventual bone loss. Unlike natural teeth, implants lack the protective mechanisms that help fight infection, making meticulous oral hygiene critical for long-term success.
Mechanical complications represent another category of potential issues. These include crown fractures, loose screws, or implant fractures—though the latter is extremely rare with modern titanium implants. Most mechanical problems can be repaired without affecting the implant itself, particularly when caught early through regular dental monitoring.
Systemic factors also influence implant success rates. Uncontrolled diabetes can impair healing and increase infection risk, while certain medications like bisphosphonates (used for osteoporosis) can interfere with bone remodeling processes. Heavy smoking significantly compromises success rates, with failure rates in smokers reaching 15-20% compared to 3-5% in non-smokers.
Medical Conditions Affecting Success Rates
Successful implant placement requires adequate bone density and volume at the implant site. Patients with severe osteoporosis may lack the bone quality necessary for reliable osseointegration, though mild to moderate bone loss can often be addressed through bone grafting procedures prior to implant placement.
Diabetes management plays a crucial role in implant eligibility. Well-controlled diabetes (HbA1c levels below 7%) doesn't significantly impact implant success rates, but uncontrolled diabetes substantially increases the risk of delayed healing, infection, and implant failure. Most oral surgeons require diabetes to be well-managed for several months before proceeding with implant surgery.
Autoimmune conditions present varying levels of concern depending on the specific disorder and treatment regimen. Conditions like rheumatoid arthritis or lupus don't automatically disqualify patients, but the medications used to treat them—particularly immunosuppressive drugs—can affect healing and infection resistance. Careful coordination between the dental surgeon and treating physicians ensures optimal timing and protocols.
Previous radiation therapy to the head and neck region can compromise bone healing capacity and requires special consideration. Hyperbaric oxygen therapy is sometimes recommended before and after implant placement in previously irradiated areas to improve healing outcomes.
Age itself isn't a limiting factor for implant placement. Healthy patients in their 70s, 80s, and beyond can successfully receive implants, provided they meet the medical and anatomical criteria. The key considerations are overall health status, bone quality, and the ability to maintain proper oral hygiene rather than chronological age.
Maintaining Dental Implants for Long-Term Success
Best Practices for Dental Implant Aftercare
Successful implant maintenance requires understanding that while implants can't develop cavities, they remain susceptible to the bacterial infections that cause peri-implant disease. Daily oral hygiene protocols for implant patients emphasize plaque removal around the implant crown and along the gum line where bacteria tend to accumulate.
The recommended cleaning routine involves specific techniques and tools designed for implant care. Soft-bristled toothbrushes or electric toothbrushes effectively clean implant crowns, while interdental brushes or water flossers help remove plaque from areas that traditional floss might miss. Many dental professionals recommend antimicrobial mouth rinses as an additional measure, particularly for patients at higher risk for peri-implant disease.
Professional maintenance visits typically occur every three to six months, depending on individual risk factors and oral health status. These visits include specialized cleaning techniques that remove bacterial biofilm without damaging the implant surface. Titanium and ceramic implant surfaces require different cleaning protocols, and dental hygienists use specific instruments designed to avoid scratching the implant materials.
Regular radiographic monitoring helps detect early signs of bone loss around implants before clinical symptoms appear. These X-rays, typically taken annually, allow dental professionals to track bone levels and identify potential problems when they're still treatable through non-surgical interventions.
Factors Influencing Implant Longevity
Research data from long-term studies reveals that properly maintained dental implants can last 30 years or more, with many implants placed in the 1960s still functioning today. The longevity depends on multiple interconnected factors, with patient compliance being perhaps the most critical variable under direct control.
Oral hygiene consistency emerges as the strongest predictor of long-term implant success. Patients who maintain excellent plaque control experience significantly lower rates of peri-implant disease and bone loss. Conversely, those with poor oral hygiene face substantially higher risks of complications that can compromise implant longevity.
Smoking represents the most modifiable risk factor for implant failure. The chemicals in tobacco smoke impair blood flow to the gums and bone, reducing the body's ability to fight infection and heal properly. Patients who quit smoking before implant placement and remain smoke-free show success rates comparable to non-smokers.
The quality of the initial surgical placement and restoration also significantly impacts long-term outcomes. Implants placed with proper angulation, adequate spacing, and optimal depth provide better biomechanics and easier maintenance access. The crown or restoration design affects stress distribution and cleanability, both crucial for long-term success.
Systemic health changes over time can influence implant longevity. The development of diabetes, autoimmune conditions, or the need for certain medications may require adjustments to maintenance protocols or more frequent monitoring. Regular communication between dental and medical providers helps address these evolving factors proactively.
Current Advances and Future Trends in Dental Implant Therapy
Innovations in Implant Materials and Technology
The dental implant field continues evolving rapidly, with recent innovations focusing on improving osseointegration speed, enhancing aesthetics, and expanding treatment options for challenging cases. Surface technology advances now allow for implant designs that promote faster bone integration while maintaining long-term stability.
Nanotechnology applications have produced implant surfaces with microscopic features that encourage specific cellular responses. These engineered surfaces can reduce healing times from the traditional three to six months to as little as six to eight weeks in optimal cases. Some manufacturers have developed surfaces that actively promote bone growth while simultaneously resisting bacterial adhesion.
Digital dentistry integration has revolutionized treatment planning and implant placement precision. Computer-guided surgery now allows for virtual implant placement before surgery, with surgical guides ensuring millimeter-precise positioning. This technology reduces surgery time, improves accuracy, and often eliminates the need for sutures.
Material science advances have produced new titanium alloys and ceramic formulations that offer improved strength while maintaining biocompatibility. Some manufacturers are exploring hybrid materials that combine the proven osseointegration properties of titanium with the aesthetic benefits of ceramics.
Expected Developments in Dental Implant Procedures
The future of implant dentistry appears increasingly focused on patient convenience and treatment acceleration. Same-day implant protocols are becoming more predictable through advances in immediate loading techniques and improved implant designs that achieve higher initial stability.
Regenerative medicine applications show promise for expanding implant candidacy to patients with insufficient bone. Techniques using stem cells, growth factors, and biocompatible scaffolding materials may eventually eliminate the need for traditional bone grafting procedures, reducing treatment complexity and time.
Artificial intelligence integration in treatment planning is beginning to analyze vast databases of successful implant cases to predict optimal placement strategies for individual patients. These systems can factor in bone density patterns, anatomical variations, and patient-specific risk factors to recommend personalized treatment approaches.
The development of smart implant technologies incorporating sensors that monitor healing progress and detect early signs of complications represents an emerging frontier. These systems could provide real-time feedback to both patients and doctors, enabling proactive interventions before problems become serious.
Conclusion
As dental implant technology continues advancing and success rates climb even higher, the question for patients facing tooth loss isn't whether implants work—it's whether they're ready to commit to the maintenance and lifestyle factors that ensure long-term success. The evidence overwhelmingly supports implants as the closest thing to natural tooth replacement available today, offering not just restored function but genuine quality of life improvements that can last decades. For those considering their options, understanding these benefits and requirements provides the foundation for making informed decisions about their oral health future.